Our retina specialists are board-certified ophthalmologists with advanced training in vitreoretinal surgery to diagnose and manage the full spectrum of diseases affecting the retina, macula, and vitreous.
Retinal Detachment & Retinal Tear
What is a Retinal Detachment/Retinal Tear
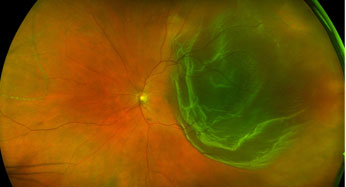
The retina is the light sensitive tissue lining the inner wall of the eye that allows the eye to see the world around you. Light rays enter the inner cavity of the eye by passing through the dark pupil at the center of your iris and strike the retina, which in a way acts like the film in a camera. This image is then sent to the brain by the optic nerve, where it is further processed into the image that you see. As light enters the eye, it passes through a clear gel-like substance called vitreous that fills the volume of the eye. As the eye ages, this vitreous gel begins to shrink and liquefy, sometimes pulling on the retina as it peels away from its surface. This is known as a posterior vitreous detachment. Most of the time, this process occurs without any problem. If there is a point of firm traction, this can result in a retinal tear or a break is formed in the delicate tissue paper like structure of the retina. Early treatment of a tear can often occur with a laser or cryotherapy probe to seal the tear. If a tear remains untreated, fluid from the inner cavity of the eye can then gain access to the space under the retina (subretinal space), causing the retina to detach from the wall of the eye. This results in a Retinal detachment, which is a vision threatening condition if not treated.
What are the symptoms of a Posterior vitreous detachment?
Flashes and floaters are the most common symptoms experienced during a posterior vitreous detachment. Any individual who experiences new flashes or floaters should have an eye exam within 1-2 days.
What are the symptoms of a retinal tear or detachment?
These symptoms are often impossible to differentiate from a posterior detachment, this is why it is important to be evaluated by an eye doctor. A curtain like obstruction of your vision coming in from the side, above, or below is particularly concerning for a retinal detachment. This is an urgent situation that should prompt you to seek immediate attention from an eye doctor.
How is a retinal tear or detachment treated?
There are a number of treatment options which may be discussed depending on the type or location of your retinal detachment.
Laser barricade
Often used for a retinal tear without detachment, or sometimes for a very small limited retinal detachment. Laser is applied while at a slit-lamp microscope, or while laying back with an indirect headlamp to surround the pathology to prevent progression.
Cryotherapy
A freezing probe is applied to the wall of the eye to create a freeze burn at the site of your retinal tear. This can be particularly useful for anterior retinal tears or if the view for laser is partially obstructed.
Pneumatic retinopexy
This is an in office procedure that may be a good option depending on the location and number of retinal tears within a retinal detachment. The retinal tears are treated with a cryotherapy probe, followed by injection of an expansile gas bubble used to tamponade the retinal tear(s) while a scar forms at the site of the tear. This procedure requires strict adherence to positioning for up to a week, which may include sleeping upright, with a head tilt, or on your side. Positioning must also continue during the day.
Vitrectomy
This is a same-day surgery that is performed in an operating room under a microscope. A combination of systemic medication and local anesthetics are used to numb the eye and keep you relaxed during the surgery. Very small port incisions are created in the wall of the eye to allow access to and removal of the vitreous gel. Fluid is drained from beneath the retina, and all retinal tears are treated with laser. A large non-expansile gas bubble is placed in the eye to provide tamponade, keeping the retina in place while the laser seals the retinal tears. You are able to go home the same day, but there are limitations on lifting >10lbs, bending over at the waist, flying in an airplane or traveling above 3000 ft with a gas bubble in your eye, avoiding getting water in the eye, and wearing an eye shield at bedtime to avoid pressure being placed on the eye.
Scleral buckle
In this same-day surgery, cryotherapy is applied to the retinal tears with or without external drainage of fluid from beneath the retina. A silicone band is sutured to the wall of the eye to apply external indentation of the sclera, in a sense creating external tamponade. This can also be performed with placement of a gas bubble. Depending on your type of retinal detachment this may be suggested as an option.
What type of vision can be expected after repair of a retinal detachment?
Many factors must be considered when discussing best corrected vision following a retinal detachment, and there is a level of uncertainty as to how much vision will be recovered. One factor is whether the macula was attached or detached at the time of diagnosis. Another factor is the length of time that the retina was detached prior to repair, or the development of scar tissue prior to repair, or following repair.
Many patients experience a drop in a few lines in vision following a retinal detachment, and while some may retain 20/20 vision, there is the potential to lose all vision in the eye despite surgical repair. The chances of recovering vision are only possible with surgery. Your prognosis is best discussed with your retina surgeon based on your circumstances.