Our retina specialists are board-certified ophthalmologists with advanced training in vitreoretinal surgery to diagnose and manage the full spectrum of diseases affecting the retina, macula, and vitreous.
Diabetic Retinopathy
In 2012, 29.1 million Americans, or 9.34% had diabetes. Of those individuals over the age of 40, .2 million (28.5%) had diabetic retinopathy. Diabetic retinopathy is a result of damage to small blood vessels in your retina caused by elevated blood sugar. Over time, elevated blood sugar causes cell death of the pericytes that line and support your small blood vessels. As these cells die, blood vessels become "leaky" and no longer are able to keep your blood and serum within the wall of the blood vessel. This results in ineffective delivery of oxygen to vital organs such as your eye.
Effects of Diabetic Retinopathy
Diabetic Macular Edema
"Leaky" blood vessels allow "fluid" to accumulate in your retina, the light responsive tissue within your eye. This is sometimes referred to by your doctor as "swelling" of your retina. This fluid accumulation causes there to be spots in your vision where things are blurry, and over time can result in a permanent drop in your best potential vision. Diabetic macular edema is a leading cause of vision loss in the United States.
Proliferative Diabetic Retinopathy
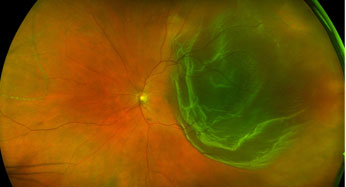
With longer exposure to elevated blood sugar, damage to small blood vessels can reduce the delivery of oxygen to your retina. The retina responds by trying to grow new blood vessels(neovascularization) in the areas affected. Unfortunately these new blood vessels have an abnormal structure, and in addition to not supplying the needed oxygen, they have a tendency to bleed into the eye causing dramatic vision loss resulting from what is referred to as a "vitreous hemorrhage." These blood vessels can also cause the retina to detach resulting in permanent vision loss. Treatment of proliferative diabetic retinopathy in a timely fashion is of the utmost importance to your vision.
Macular Ischemia
As blood/oxygen supply to your eye is diminished over time, it can have a profound effect on your vision, essentially starving your retina of its necessities to survive, resulting in permanent cell death. This can cause an irreversible loss of your central vision.
Treatment of Diabetic Retinopathy
Panretinal Photocoagulation
This is a method of turning down the signal your retina sends out to create new blood vessels. It involves the placement of laser burns in the peripheral retina in a pattern that reduces the production of a molecule referred to as vascular endothelial growth factor (VEGF). By turning down this signal, this type of laser is used as a treatment for proliferative diabetic retinopathy, as well as a number of other eye conditions that result in neovascularization, or new blood vessel growth.
Focal/Grid Laser
This is the use of low power laser burns to treat macular edema. This is felt to stimulate the retina to reduce retinal swelling through the production of a molecule known as heat shock protein. This can be a very helpful adjunct to other treatment options, but requires the source of fluid leakage to be a certain distance from your central vision for use of the laser.
Anti-VEGF Medication Injections
These medications target the VEGF molecule by directly binding and preventing its deleterious effects on the retina. These medications include Avastin(bevacizumab), Lucentis(ranibizumab), and Eylea(aflibercept). These medications have revolutionized the treatment of certain eye conditions, including diabetic retinopathy, age related macular degeneration, retinal vein occlusions, and others. Although they are very effective, the medication only has a certain half-life and usually requires repeat treatments to control your eye disease.
Intraocular Steroids
Steroids are another effective treatment for macular edema. There are a number of delivery systems including Triesence, Ozurdex, and Iluvien. Careful discussion is required with your retina specialist to determine what is the best treatment option for you.
Educational Video
Online Resources
- Diabetic Retinopathy - The National Eye Institute
- What Is Diabetic Retinopathy? - American Academy of Ophthalmology